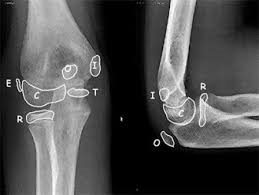
Orthopedics Outcome- case #3
Posted on: July 26, 2016, by : Jennifer Chapman
Diagnosis: medial epicondyle fracture with fragment retained in joint. This is the third most common pediatric elbow fracture.
The subtle finding is that the radius and ulna are not in a correct position (subluxated)– the AP view shows the radius to be out of alignment with the capitellum, even though the lateral view shows good positioning. Subtle and can be missed, since we tend to look primarily at the lateral view for alignment.
Responses from PEM readers:
Diagnosis: (14 votes) Epicondyle fracture (64%) Condyle fracture (21%) Type 1 SCFx (15%)
Is Orthopedic consult needed in ED: Yes = most, with 1 vote for longer f/u
Our Orthopedic colleague responds:
Clinical pearls:
- Mechanism and typical age: this injury is seen in school age (~7yo) to adolescence. Mechanism of injury is a valgus force on the elbow (forearm forced in thumb’s direction with elbow as fulcrum). This can occur with a single traumatic episode, such as falling back onto the hand in a backbend posture, or with repetitive injury, such as pitching. In the latter, the medial epicondyle fracture does not generally have any associated injuries; there is often a history of medial elbow pain weeks to months prior elicited in that circumstance.
- Anatomy: the medial epicondyle of the elbow is a prominence on the inside/medial aspect of the distal humerus. It is an apophysis onto which tendon and ligament inserts. When a fracture occurs through an apophysis, it can be more difficult to appreciate as the fracture line itself passes through a cartilaginous structure that cannot be seen except as a dark line on plain film imaging. However, if one appreciates that there should be an epicondyle present medially and it is not visible, this should prompt further evaluation with plain film and may prompt obtaining contralateral films.
- Almost 1/2 of these fractures are associated with elbow dislocations. Some of these dislocations spontaneously reduce and the full nature of the injury can be missed in this situation. The greatest risk posed is when the medial epicondyle becomes incarcerated within the elbow joint and this goes unnoticed. This occurs when there is no clear fracture line present (see discussion of apophyseal fractures above). Again, searching for the structure in the joint or obtaining contralateral x-ray may be useful in this situation.
- On clinical exam, there is usually a lot of swelling and even ecchymosis over the elbow or proximal forearm, and tenderness over the condyle, often medially and posteriorly.
- Diagnostics: Order 3 views of the elbow when assessing trauma. If a medial epicondyle fracture is suspected, add an EXTERNAL rotation oblique. If a lateral epicondyle fracture is suspected (much less common), add an INTERNAL rotation oblique. (this can be added in the comments section in Cerner).
- Radiology: the medial epicondyle generally has ossified and is visible on x-ray by 5 years of age. This is part of the CRITOE mnemonic to identify normal and malpositioned structures
7. Dispo: If non-operative management is chosen, a well-padded long arm posterior splint just past the wrist can be applied. Some orthopedic surgeons prefer flexion to be held at 30 degrees or at 90 degrees with the forearm pronated.
8. Follow-up in 5-7 days is a reasonable timeframe for non-operative epicondyle fractures.
Red flags requiring Orthopedic consult in the ED:
- Absolute indications for operative management are open fractures and medial epicondyles incarcerated in the joint. Look for joint incongruity on AP and lateral imaging. An elbow can appear to be reduced on the lateral and still be translated on the AP or vice versa.
- Consider consultation in ED if the fracture is displaced greater than 5mm or associated with an elbow dislocation, even if the dislocation was reduced and the fragment is not incarcerated. Fracture displacement in these cases is often significantly underestimated so be sure to evaluate the displacement on ALL images. In light of this, consider obtaining ED consultations for all but entirely non-displaced medial epicondyle fractures.
_______
Pattern recognition:
These are Xrays of different patients. Identify any injury: (see answers below)
[embeddoc url=”https://pemacademy.com/wp-content/uploads/2016/07/Elbow-fx-patterns-3-1.pptx” download=”all” viewer=”microsoft”]
Case 1: adolescent fall during sports: medial epicondyle fracture with fragment incarcerated in joint. Arrow points to anterior elbow effusion.
Case 2: adolescent fall during sports: medial epicondyle fracture with fragment incarcerated in joint
Case 3: adolescent overuse injury ending with sudden ‘pop’, now with medial epicondyle fracture.
Case 4: school-aged child with fall on outstretched hand (FOOSH), now with displaced radial neck fracture and non-displaced olecranon fracture.
Case 5: capitellum, radial head, and internal/medial epicondyle visible. It is reasonable to estimate this child at older than 5 years and younger than 7 years (no trochlea visible).