Hot Seat #190: Umbilical Uncertainty
Posted on: May 11, 2022, by : Walter Palmer
HPI:
16-day-old ex-38 wk male who presents with erythema around the umbilicus.
The umbilical stump fell off 1 day ago, and since last night parents have noticed redness along the umbilicus. This morning the erythema has worsened and child seems to be fussy upon touching the umbilicus. No drainage or pus from umbilicus. No fevers at home and has been acting per baseline, tolerating PO well and although intermittently fussy, is consolable.
ROS:
Constitutional symptoms: Denies fever.
Skin symptoms: denies jaundice, denies rash, denies diaper rash. + erythema around umbilicus.
Eye symptoms: denies discharge, denies redness.
ENMT symptoms: denies nasal congestion.
Respiratory symptoms: denies cough, denies stridor, denies cyanosis.
Gastrointestinal symptoms: no vomiting, tolerating PO well
Genitourinary symptoms: no hematuria
Neurologic symptoms: fussy but consolable
Allergy/immunologic symptoms: no impaired immunity.
PMH:
Ex38wkr, C/S , GBS negative, no NICU stay. G6PD+ on NBS.
Vaccinations: Hepatitis B and Vitamin K at birth.
SH: Lives with both parents.
Meds: No home meds, none given prior to presentation.
Exam:
VS: 37.8 C (rectal), HR: 166, RR: 36, BP: 95/58, SpO2: 100%
General: Alert. Appropriate for age.
Skin: Warm. dry. intact. See GI for umbilicus description.
Head: Normocephalic. atraumatic. anterior fontanelle soft and flat.
Eye: Pupils are equal, round and reactive to light. extraocular movements are intact. normal conjunctiva. no discharge.
Ears, nose, mouth and throat: Oral mucosa moist. No pharyngeal erythema or exudate.
Cardiovascular: Regular rate and rhythm. Normal peripheral perfusion. Extremity pulses equal.
Respiratory: Lungs are clear to auscultation. respirations are non-labored. breath sounds are equal.
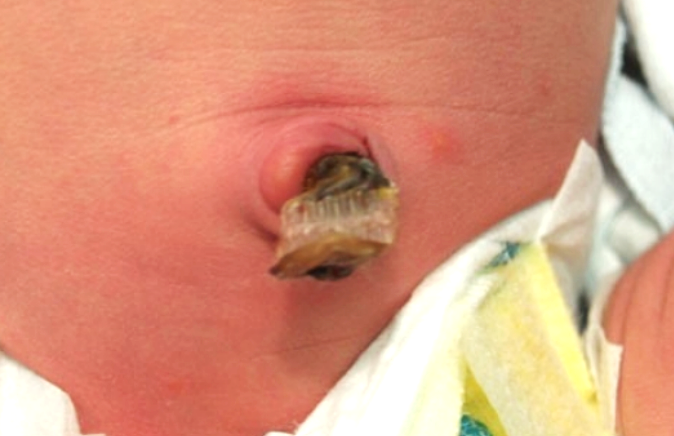
Gastrointestinal: Soft. Nontender. Non distended. + reducible umbilical hernia, tip of umbilicus is erythematous w/ mild duskiness of superior aspect of umbilicus, no purulence or fluctuance.
Genitourinary: Normal genitalia for age.
Back: Normal range of motion. Normal alignment.
Musculoskeletal: Normal ROM. normal strength. no deformity. moves all extremities.
Neurological: Alert. Moves extremities spontaneously, symmetric Moro reflex
Labs were obtained including: CBC, Inflammatory markers, blood culture and UA. LP was deferred given lack of true fever and general well appearing status on presentation.
CBC: 18.52<11.6/33.4>438
Inflammatory markers: CRP 0.81 (Threshold: 1.5), Procalcitonin 0.10 (Threshold 0.10), ESR 12 (Threshold 20)
UA: Nitrite neg, LE negative, 4 WBC, No bacteria
Given presumably worsened erythema and borderline labs, decision was made to admit to Hospitalist and start IV antibiotics for next 24 hrs for observation and pending growth of blood culture.

Le sigh. The ambiguity. I wish this kid would just spike a fever already! Stay outside or come inside. All this door swinging is letting in flies.
Omphalitis is a scary illness, and I like to sleep at night, so many things have to be present/absent for me to send you home. You have to look amazing other than the erythema (this kid is slightly fussy), it has to be completely nontender (both on history and exam), and obviously you need to be afebrile (this kid is skating around a fever). So…this one needs to be admitted.
In terms of whether to do a full septic workup or not–if the kid was absolutely inconsolable or unambiguously febrile, obviously a full septic workup would be appropriate. If this were 15 years ago, we’d be having a lot longer discussion about what to do. But in 2022, I think a CBC, procalcitonin, and CRP are the way to go in trying to make a decision about a full sepsis workup. Let’s remember that often in the NICU, afebrile/non-hypothermic kids who have other reasons for us to suspect sepsis have been getting only a CBC, blood cx, CRP, and 48 hour/7-day rule out sepsis with antibiotics on board for a while now. So in this kid, I think that’s appropriate; I might not have even included the UA. I don’t love the fact that the WBC count is 18, and that may have made me want to tap the kid. But in a meta-analysis published in the journal Critical Care in 2018 (doi: 10.1186/s13054-018-2236-1), CRP + procalcitonin had a pooled sensitivity of 0.91 (0.84, 0.95) and a negative likelihood ratio of 0.1 (0.05, 0.19). (The NLR makes me feel a bit better about potentially missing ~9% of the kids.
Also, a test called presepsin seems to have even better numbers.) I have no issues using the PCT and procal in a kid like this IF I’m going to admit them. It would not be enough for me to send them home untapped. Not yet. Maybe presepsin will allow me to sleep at night.
There was a nice PEMCRC study just published in the current issue of Pediatrics to address omphalitis and concurrent SBI (DOI: 10.1542/peds.2021-054189).
Conclusion: “In this multicenter cohort, mild, localized disease was typical of omphalitis. SBI and adverse outcomes were uncommon. Depending on age, routine testing for SBI is likely unnecessary in most afebrile, well-appearing infants with omphalitis.”