Hot Seat #191: A Pain in the Neck
Posted on: May 23, 2022, by : Brian Lee
Case by: Jessica Hippolyte, MD, MPH
You are carrying THE phone when you get a call from EMS regarding destination decision. They are on scene with a 7 year-old who was a restrained backseat passenger who was involved in a front end MVC. Unclear speed of oncoming vehicle (patient’s vehicle was going ~15mph). Patient was ambulatory at scene, but is currently complaining of neck pain with an associated linear ecchymosis where his seatbelt was fastened.
In a conversation with you, EMS and local hospital, the decision was made to bring the child to a pediatric trauma center.
HPI: 7-year-old male with asthma who presents to the ER following a motor vehicle collision that occurred 2 hours prior to arrival. Patient was a restrained backseat passenger with no loss of consciousness and no head injury. The collision resulted in airbag deployment, but no major injuries reported at the scene for any other passengers. The vehicle speed was unclear but thought to be around 10-15mph. Patient reports being ambulatory at the scene. He presents to the ER with anterior neck pain around the area where the seat belt laid on his neck.
PMH: asthma
PSH: none
Meds: none
Allergies: none
Immunizations: up to date
EXAM
Vitals: T-36.8, HR-94, RR–20, BP 118/68, SpO2 99% on RA
General: Alert. NAD. appropriate for age
Skin: Warm. No rash. Shallow abrasion and erythema over right anterior neck, no bruising
Head: Normocephalic. atraumatic.
Neck: Immobilized in rigid collar; trachea midline, no swelling, no hematoma, no crepitus. + anterior neck pain with associated eccymosis, worse to palpation (see picture below).
Eye: PERRL, EOMI. Normal conjunctive.
ENT: Facial bones intact. No oral trauma
CV: Regular rate and rhythm. Normal S1/2. No murmur. Normal peripheral perfusion. Extremity pulses equal.
Resp: Lungs are clear to auscultation. Respirations are non-labored. Breath sounds are equal. Symmetrical chest wall expansion.
Chest wall: No crepitus, + b/l clavicular pain with no deformity
Back: Nontender. Normal range of motion.
Musculoskeletal: Normal ROM. No deformity. Moves all extremities.
Gastrointestinal: Soft. Nontender. Non distended. No bruising
Neurological: GCS 15, alert with no focal neurologic deficits, Cranial nerves II – XII: intact. 5/5 motor strength upper and lower extremities bilaterally, intact sensation
Skin/Neck:
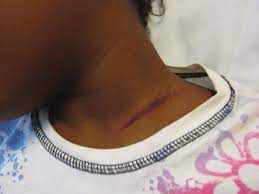
Patient receives Tylenol for pain control. Workup notable for normal bilateral clavicle radiographs. Basic trauma labs (UA, Hemoglobin, AST/ALT) unremarkable. Vitals remain stable (HR 90, RR 18, BP 111/74).
On exam to clear c-spine: denies pain with palpation over each cervical vertebrae, full ROM of neck (side to side, up/down). Endorses anterior neck pain, worse to palpation.
Image Credit: Desai NK et al. “Screening CT Angiography for Pediatric Blunt Cerebrovascular
Injury with Emphasis on the Cervical ‘Seatbelt Sign.’” American Journal of Neuroradiology. 2014; 1836-1840.
The information in these cases has been changed to protect patient identity and confidentiality. The images are are only provided for educational purposes and members agree not to download them, share them, or otherwise use them for any other purpose.

Are we to factor in the international shortage of CT contrast currently in making our decision regarding to CTA or not?
In all seriousness, getting a neck CTA for all lapbelt-induced cervical abrasions is probably not necessary. Clearly if there are definite signs of a blunt cerebrovascular injury (cervical/facial arterial hemorrhage, expanding cervical hematoma, cervical bruit, focal neurological deficit) or clear risk factors (severe injuries such as midface/mandibular fracture, complex skull/facial fractures, TBI with thoracic trauma, TBI requiring intubation, injuries on C-spine imaging, hanging induced anoxic brain injury, upper rib fractures), then we should get a neck CTA. Also, if there is “significant swelling, pain, or altered MS” (UpToDate; Blunt cerebrovascular injury: Mechanisms, screening, and diagnostic evaluation) then neck CTA should be obtained.
So, for this case, all there really is “pain” at the site of the abrasions. Here, getting a neck CTA is really a judgment call — one that, I argue, could be facilitated by a good physical exam. One needs to decide if the pain at the abrasion is secondary to the abrasion (which can be quite painful) or is secondary to damage to deeper vascular structures. Things to try: (1) pinch the abrasion and see if all the pain is superficial, (2) move the abrasion laterally and palpate under where the abrasion used to be for deeper tenderness, (3) put a little LET on the abrasion to see if that takes most/all of the pain away (which argues for superficial injury). My hunch is that almost all cervical lapbelt abrasions in kids will be superficial and not require a CTA — despite many of us ordering CTAs for these!